This week we released a new study, “2019 Women's Health and Oncologist Workforce Analysis” which details the growing shortage of U.S. oncologists and the serious impact it may have on women’s healthcare.
Breast and lung cancer are the top two leading cancer-related deaths for American women. With this in mind, the American Society of Clinical Oncology (ASCO) is also projecting a shortage of over 2,200 oncologists over the next six years.
In order to understand the severity of the shortage and its potential impact on cancer patients, we examined more than 18,000 Doximity profiles of full-time, board-certified oncology practitioners. In this newly published study, we have uncovered the top 10 MSAs that will most likely to suffer a shortage of oncologists in the coming years.
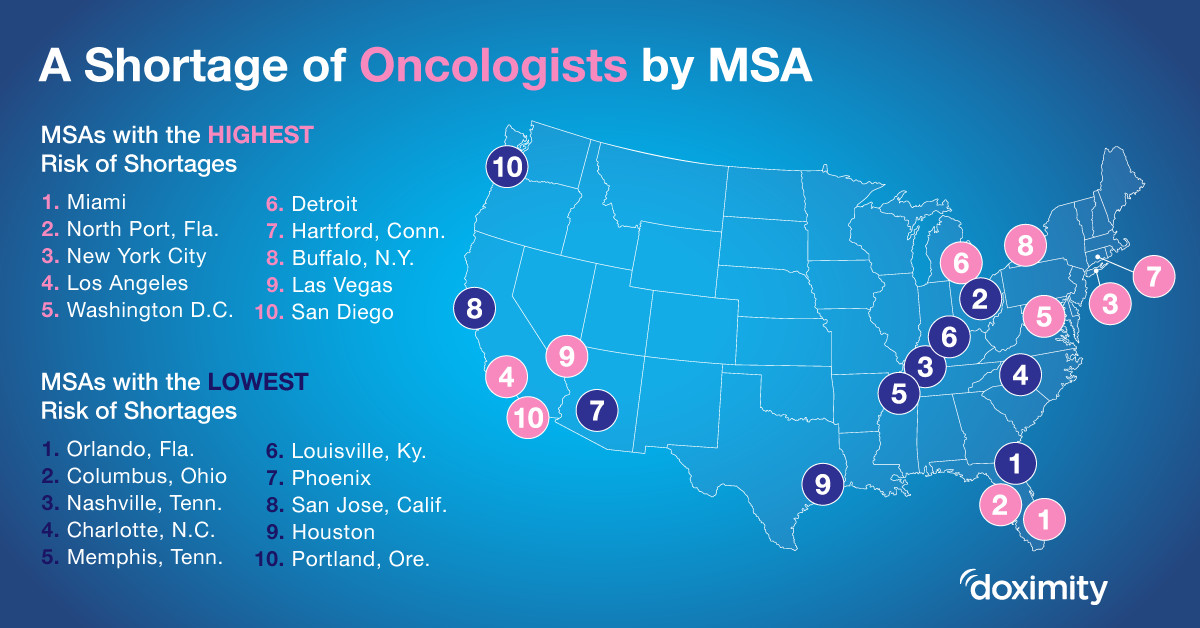
With Miami ranking number one on the list, we asked local oncologists for their thoughts on this troubling trend. Dr. Jose Lutzky in Miami Beach shares, “The impact of these demographic trends is already being felt in the Miami-Dade area as it has become quite difficult to recruit younger oncologists to replace retiring physicians. Other compounding factors that contribute to the shortage are the high cost of living and impossible traffic in Miami-Dade county. In order to accommodate cancer patients that need to be seen soon and/or frequently, oncology practices will need to resort to extended hours, further increasing the stress on physicians and ancillary personnel.”
Also based in Miami Beach, Dr. Mike Cusnir explains further the severity of the shortage. “Overall, there are several competing factors that we are seeing as concerns for the shortage in oncologists in our area. There has been some consolidation of the providers under the large hospital systems with a rapid decline of the private practices in the area. The main concern is that even as the medical director of one of the cancer centers in one of largest hospitals in the area (only one in Miami beach) we have not been very successful in recruiting for many reasons."
Dr. Cusnir continued, "One reason being that the pay gap between academia and private practice has narrowed, but moreover the pay differential for an area with a high cost of living has not changed much by comparison in other areas. All of this is worsened by the increase in the number of patients that we are seeing secondary to the increase in insured patients after the introduction of the health care act (Obamacare). Lastly, our area has a high level of malpractice lawsuits that prompts the primary care practitioners to practice defensive medicine, which in turn increases referrals to specialists.”
To view the full report, please click here.
